2026 Medicare Parts A & B Premiums and Deductibles

Updated for the 2026 Plan Year
On November 14, 2025, the Centers for Medicare & Medicaid Services (CMS) released the 2026 premiums, deductibles, and coinsurance amounts for Medicare Part A, Medicare Part B, and the 2026 income-related monthly adjustment amounts (IRMAA) for Medicare Part D.
Part A (Hospital)
Inpatient Hospital Stay – You Pay … (benefit period ends 60 days after release from care)
- Deductible: $1,736 per benefit period
- Coinsurance (days 1-60): $0 per day of each benefit period
- Coinsurance (61-90): $434 per day of each benefit period
- Coinsurance (60 Lifetime reserve days): $868 per day after day 90 of each benefit period
Skilled Nursing Facility Stay – You Pay … (3-day inpatient hospital stay required first)
- Coinsurance (days 1-20): $0 per day of each benefit period
- Coinsurance (days 21-100): $217 per day of each benefit period
Part B (Medical)
- Part B Deductible – You Pay … $283 per calendar year
- Part B Coverage – Your Pay … Generally 20%, after $283 deductible is met
Part B Premium (including high-income Part B & Part D) [paid to Medicare]
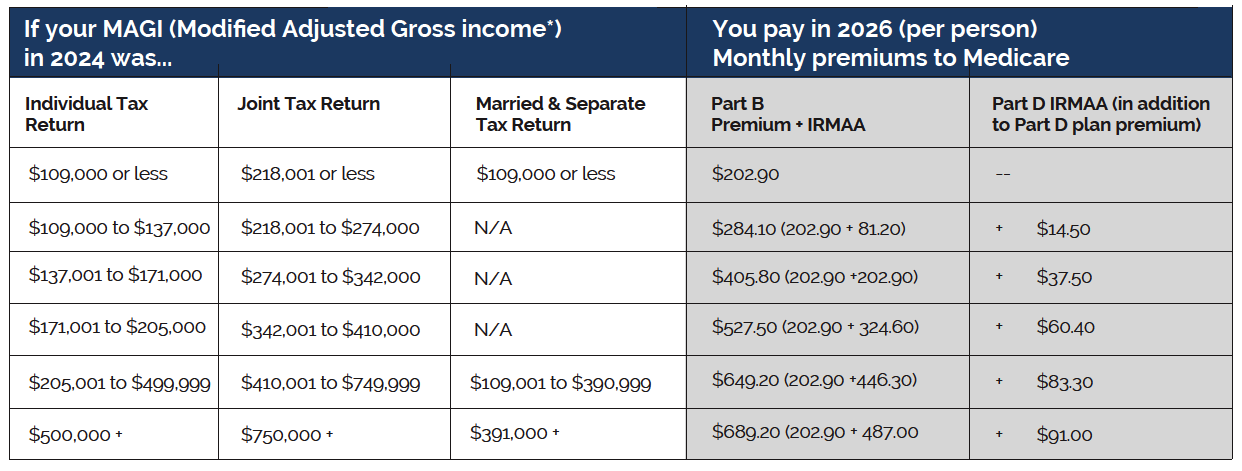
Those enrolled in Part B will pay at least the standard $202.90/mo premium (based on income). Higher income earners will pay a Part B IRMAA (Income Related Monthly Adjustment Amount) in addition to the $202.90/mo standard premium.
Higher income earners who are enrolled in Part D Prescription Drug coverage also pay a Part D | IRMAA in addition to the monthly insurance premium for a Part D prescription drug plan or Medicare Advantage plan that includes Part D coverage (see table below).